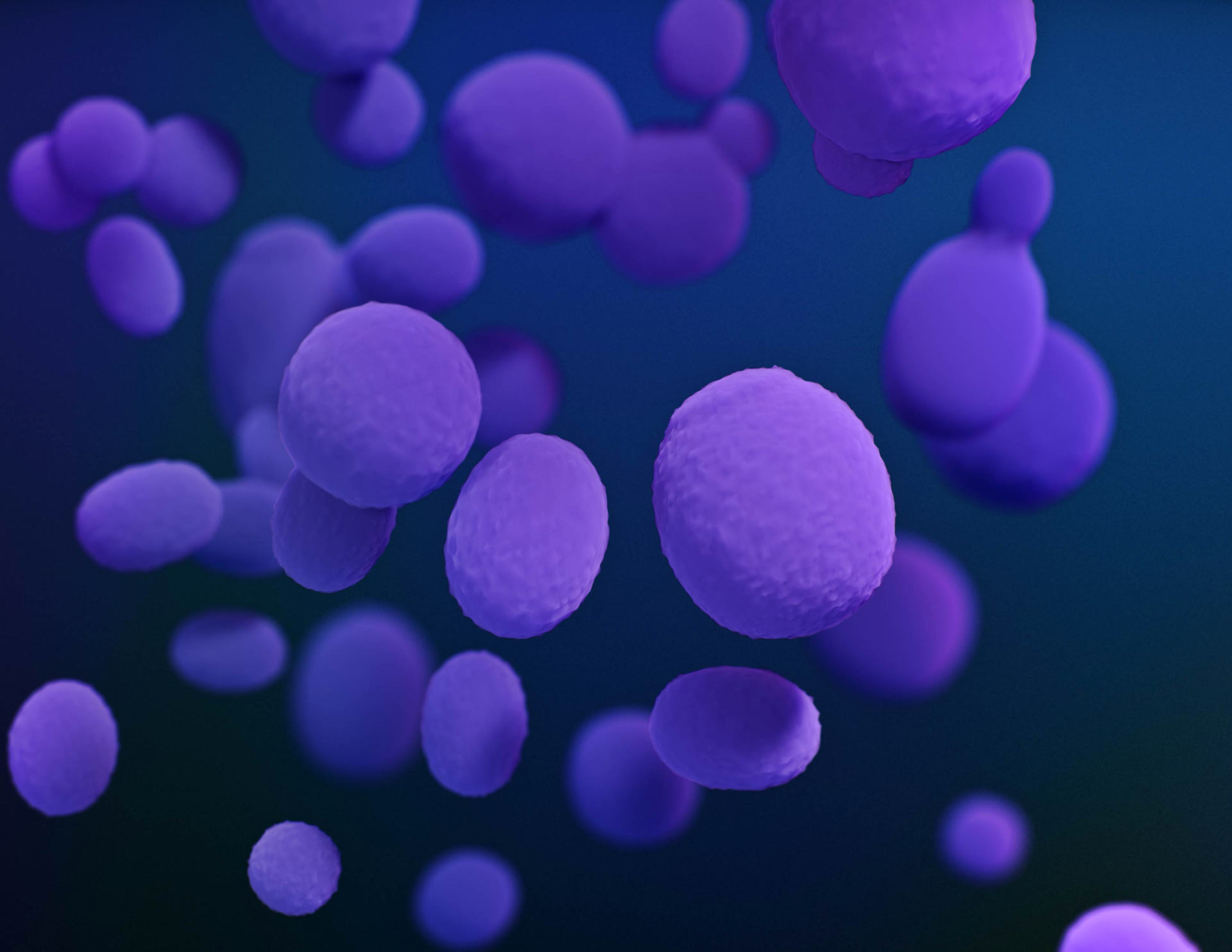
A new study in mice shows that normally, the immune system keeps potentially pathogenic fungi such as Candida albicans in check, targeting them when they switch into a state that can cause harm; when the system is off-balance, disease is more likely to occur.
Candida albicans. Image credit: Stephanie Rossow / Antibiotic Resistance Coordination and Strategy Unit, CDC.
“Fungi have been wholly understudied in part because they are vastly outnumbered by bacteria,” said senior author Professor June Round, a researcher in the Department of Pathology at the University of Utah School of Medicine and the Huntsman Cancer Institute at the University of Utah.
“New tools and technologies are starting to make investigations like this one possible.”
Professor Round and colleagues became interested in this line of research after noting that a common medical test for diagnosing Crohn’s disease, a type of inflammatory bowel disease, works by detecting antibodies against fungi.
And yet, how antibodies affect fungi’s influence on disease had yet to be explored.
To dig deeper, the researchers searched for the trigger of the immune response.
Working with patient samples and carrying out tests with mice, they determined that Candida albicans elicited the strongest immune response.
Further investigation showed that antibodies zeroed in on elongated fungal cell types called hyphae, specifically binding to proteins called adhesins that help microbes stick to surfaces and become invasive.
With this target in hand, the scientists could more definitively probe the fungi’s role in gut health.
They found that mice populated with Candida albicans in its normal, rounded state remained healthy.
In contrast, mice populated with the yeast in its invasive form caused intestinal damage that resembled inflammatory bowel disease.
The results show that normal antibody responses in the gut inhibit disease by recognizing the harmful, hyphal form of fungi.
Inflammatory bowel disease isn’t the only health condition associated with fungi. Another is vaginal yeast infections.
The researchers determined that a vaccine being investigated as a remedy for yeast infection triggered an immune reaction against adhesin proteins that is similar to the reaction in Crohn’s patients.
When inoculated with the vaccine, mice normally prone to an inflammatory bowel disease-like condition were less likely to develop disease.
“We aim to exploit interactions with commensal microbes and the host immune system to harness microbial products for therapies,” Professor Round said.
In addition to implications for disease, the findings also suggest fungi may be important in the healthy gut.
Typically, the immune system’s job is to clear infections by getting rid of invasive organisms. In this case, fungi benefit from their interaction with antibodies.
The immune reaction prods fungi from their invasive state into their rounded, budding state, which improves their survival in the gut.
“The immune system is constraining Candida to its least pathogenic form,” said first author Dr. Kyla Ost, a postdoctoral researcher in the Department of Pathology at the University of Utah School of Medicine and the Huntsman Cancer Institute at the University of Utah.
“This is showing us that the communication between host and microbe can be friendly, as opposed to antagonistic, in order to benefit both.”
The study was published in the journal Nature.
_____
K.S. Ost et al. Adaptive immunity induces mutualism between commensal eukaryotes. Nature, published July 14, 2021; doi: 10.1038/s41586-021-03722-w
 #Bizwhiznetwork.com Innovation ΛI |Technology News
#Bizwhiznetwork.com Innovation ΛI |Technology News